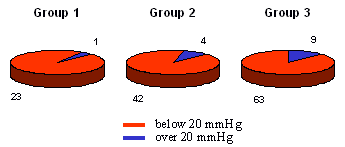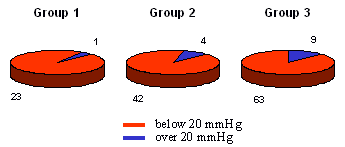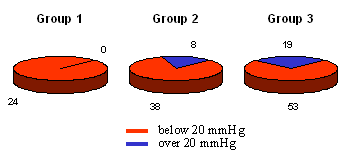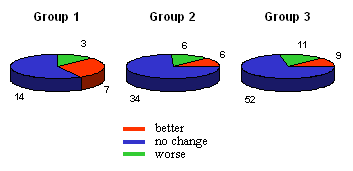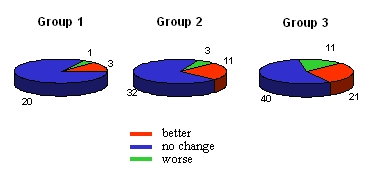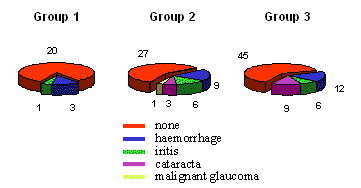The Role Of Trabeculectomy In The Treatment Of Glaucoma: Predicting the
Need For Surgical Intervention
In the treatment of glaucoma, surgical intervention is considered
as a last resort, which should be performed only after an unsuccessful
medical treatment. This view is based on three main arguments:
-
There is wide and expanding range of possibilities for medical treatment
-
As opposed to other surgical interventions, anti-glaucoma operations are
not followed by immediate and impressive change of the visual functions.
-
By itself, the intraocular tension reduction reached by the operation will
not always halt the progress of glaucoma.
Because of these, doctor and patient will initially reject surgical intervention.
However, surgery will eventually be inevitable, and it will take place
at the time when serious functional damage has already developed. This
explains
the reason why the recent years' literature contains so few references
on trabeculectomy, that are useful for statistical purposes. A rare exception
is Alemu's over 400 cases in Ethiopia.
At the Eye Department of Saint John Hospital, Budapest 169 trabeculectomy
were performed during the last 4 years, and of these 142 patients were
followed for at least one year. The patients were classified in three groups,
based on the severity of visual field defect. The patients with none or
minimal visual field defect are in group 1. Those with medium visual field
defect are in group 2, and group 3 contains the ones with severe
visual field defect. (Table 1)
|
Group 1 |
Group 2 |
Group 3 |
| Number of patients |
24 |
46 |
72 |
| Sex (male/female) |
7/17 |
16/30 |
31/41 |
| Average age |
60.6 |
65.9 |
73.7 |
| Age |
52-68 |
46-79 |
32-87 |
Table 1.: The patient groups
All of the operations were performed by the same surgeon using the same
method: limbus based conjunctival flap and wide basal iridectomy through
the trabeculectomy.
Of the 142 patients, 16 had narrow angle glaucoma and 126 had open
angle glaucoma (of these 12 cases with pseudoexfoliation) . With the exception
of three, all patients were subject to earlier medical treatment for several
week, months or even years. They all had incorrigibly high intraocular
tension before the operation.
The surgical intervention was considered successful if the intraocular
tension dropped below 20 mmHg.
Figures 1 and 2 show the intraocular tension 6 weeks and one year after
the operation. While the patients in the first group had normal intraocular
tension after one year, the patients in the third group had suffered a
setback after the initial good results. Practically this meant that for
these patients in was necessary to restart medical treatment.
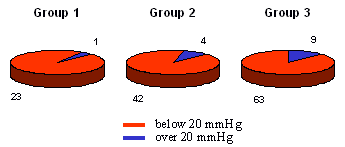 |
| Figure 1.: IOT 6 weeks after operation |
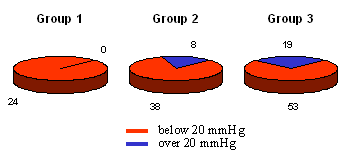 |
| Figure 2.: IOT one year after operation |
The change in the visual acuity is similar: in group 1 the visual acuity
improved in more cases than in which it decreased. however, in group 3
there were only few cases with improved visual acuity. (Figure 3).
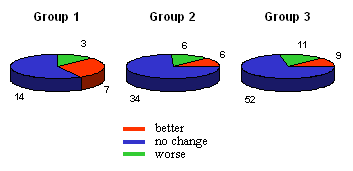 |
| Figure 3.: Visual acuity one year after operation |
The most promising results were achieved with the visual field. The
number of patients with improved visual field is much higher than the number
of cases with worse result. This is specially true for group 3. (Figure
4).
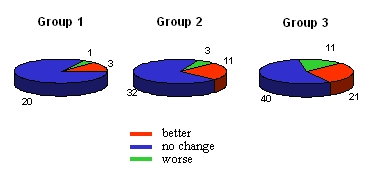
|
|
Figure 4.: Visual Field 6 weeks after operation
|
For these patients the improvement in the visual field was not only
measurable but visible for the patient also. See visual
field charts.
Most of the early complications of the surgery were haemorrhage in
the anterior chamber and iritis, while later cataract was common (Figures
5 and 6). While cataract may be of serious concern for the patient and
the doctor, it can be surgically treated at a later time. After the successful
lens implantation, patients have experienced large scale improvement, even
in the case of group 3.
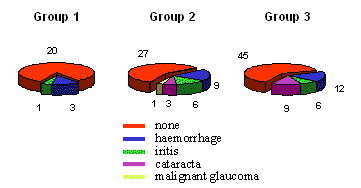 |
| Figure 5.: Complications after 6 weeks |
 |
| Figure 6.: Complication after 1 year |
If the success of the surgery is defined as the reduction of intraocular
tension, than surgical intervention performed on patient group 1 were in
100% successful. In group 2 the percentage of success is 82%, and in group
3 it is 73%.
Thus we can safely assume, that in certain cases the surgical treatment
of glaucoma can be used as a first treatment.
If surgery is used at the time of large scale functional damage, after
an unsuccessful medical treatment, then the results are not so good. This
also means, that the sooner the decision is made for surgery, the better
the results will be.
During a retrospective analysis of our surgical cases, we were collecting
those symptoms, that indicate the necessity of a surgical intervention.
Based on the results obtained, a scoring table were developed to predict
the need for surgery after glaucoma attack (Table 2) and primary glaucoma
(Table 3)..
| Symptoms |
Score |
| Pupil remains dilated |
1 |
| Pupil irregular |
1 |
| IOT over 24 mmHg |
2 |
| IOT borderline |
1 |
| Chamber angle mainly closed |
1 |
| Surgery if total score is at least |
2 |
Table 2.: Predicting the need for surgery
after glaucoma attack
| Symptoms |
Score |
| Initial IOT > 30 mmHg |
1 |
| IOT often over 24 mmHg during medical treatment |
1 |
| Pathological chamber angle |
1 |
| Visual field defect |
2 |
| Optic nerve head excavation |
1 |
| Maximal medical treatment |
2 |
| Age below 50 |
1 |
| Low blood pressure |
2 |
| Myopia |
1 |
| Surgery if total score is at least |
4 |
Table 3.: Predicting the need for surgery
for open angle glaucoma
Assessing a glaucoma case by this scoring system at the time of first
diagnosis or at any later time, decision can be made to continue medical
treatment and risk further deterioration or perform - a possibly inevitable
- surgery as soon as possible.
To summarize:
-
Surgery is a viable first treatment for glaucoma
-
The sooner this surgery is performed, the less complication will arise,
with greater chance of complete success.
-
The scoring system described in this paper is able to predict the need
for surgical intervention with great probability.
Finally, the problems associated with the surgical treatment of glaucoma
are well illustrated by the following:
One of our patient (with very high initial IOT) said when he lost his
vision due to cataract developed after a trabeculectomy: "Doctor, you only
needed 20 minutes to do what nature would need months for". He immediately
changed this opinion, with great joy, after a successful lens implantation
later.
This means that all complications of a glaucoma surgery can be remedied
after the intraocular tension is normalized, but no functional damage developed
during an insufficient medical treatment be redone.
|
Discussion
Board|
Next
Page|
Your
Symposium|