Medicine Poster Session
| INABIS '98 Home Page | Your Session | Symposia & Poster Sessions | Plenary Sessions | Exhibitors' Foyer | Personal Itinerary | New Search |
Introduction
The clinical manifestations of sickle cell disease (SCD) are produced by the biochemical mechanism of a single base substitution of valine for glutamic acid in position 6 of the ß-hemoglobin subunit HbA[ß6val] --> HbS[ß6glu]). In the deoxygenated state, this mutation results in a distortion, or "sickling" of the RBC, which is responsible for the vaso-occlusive crises that characterize SCD pathology. SCD is endemic to peoples of African descent, both northern and sub-Saharan, as well as certain populations of the Mediterranean Basin and India.1-3 The high frequency of the HbS allele among these populations arose from the selective advantage the heterozygous genotype (HbAS) provides against malarial infection.3 Competing models exist to explain the fact that the malaria parasite does not survive well in the RBC's of the HbAS (trait) host compared with the HbAA host. In non-tropical regions without malarial pressure such as the United States, no survival advantage is believed to be afforded sickle cell trait and, therefore, the relevant clinical medical issue becomes the management of the SCD population. As might be expected, the combined stress of SCD and pregnancy can have profound implications for maternal and fetal morbidity.4 Previous studies exploring pregnancy outcomes in sickle cell patients have reported increased incidence of spontaneous abortion, pregnancy-induced-hypertension, infections, pre-term labor, and low birth weight.5-7 Studies have also been conducted to ascertain whether trait women might also be at increased risk for some of the same pregnancy issues.8 The purpose of this study was to assess the quality of pregnancy outcomes among a cohort of African American women with and without hemoglobinopathies who delivered at the University of South Alabama Medical Center (USAMC) for the years 1991-1996.
Materials and Methods
Several electronic databases were cross-linked to develop our research database covering a period from June 1991 to June 1996. 23,000 deliveries existed in an electronic database at the USAMC Department of Obstetrics and Gynecology (OBGYN) for this period. The USAMC database was accessed to determine hemoglobinopathy status using ICD9 codes. Hemoglobinopathy status was checked for accuracy and completeness with MEDICAID and USA Sickle Cell Center databases. The latter identifies most of the local SCD population. The OBGYN records were cross-linked with the diagnostic database resulting in 11,845 births to 9,310 African American women, with 21.4% repeat births. We selected last birth for each woman in the five year period and the firstborn of each twin pair resulting in a sample of 9,310 deliveries consisting of (1) homozygous SCD, n=50, (2) heterozygous HbAS trait, n=336, (3) other hemoglobinopathies, n=29, (4) HbAA population, n=8,895. Data selected for study included age, gravidity, gestational age, birth weight, infant sex, perinatal death, apgar scores, anemia during pregnancy, toxemia and hypertension, diabetes, and infection. Database management was performed using EXCEL. These data were then imported into a SYSTAT database format for univariate and multivariate statistical analyses.9 Statistical tests performed on the data included t-test, chi-square, and stepwise multiple linear regression and multiple logistic regression analyses. For the sake of brevity statistical comparisons and discussions presented here were restricted to HbAA and HbSS women for selected data.
Results
Women in the study were from a lower socioeconomic background and part of the USAMC MEDICAID population. Fetal (prenatal + perinatal) loss was significantly more prevalent among HbSS mothers (fig. 1)
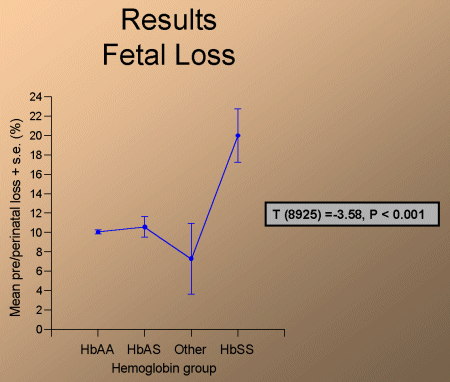 Fig. 1: Fetal loss rate.
Fig. 1: Fetal loss rate.
as was pregnancy-induced hypertension (fig 2).
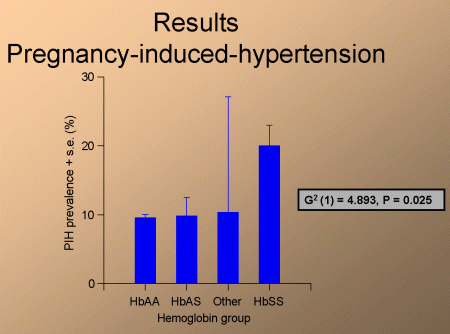 Fig. 2: Pregnancy-induced hypertension.
Fig. 2: Pregnancy-induced hypertension.
Prevalence of pyelonephritis was significantly higher among HbSS women (fig. 3).
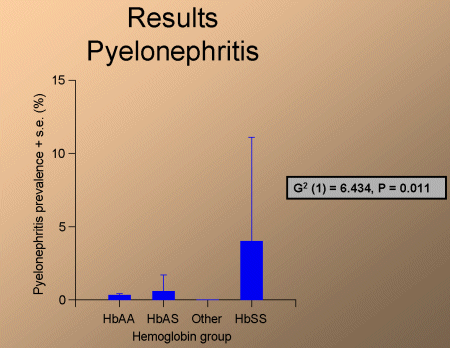 Fig. 3: Pylelonephritis.
Fig. 3: Pylelonephritis.
HbSS women delivered significantly earlier than HbAA women (fig. 4)
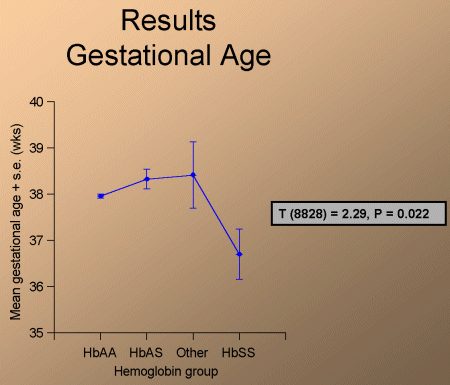 Fig. 4: Gestational age.
Fig. 4: Gestational age.
and birth weights were significantly lower for their neonates (fig. 5).
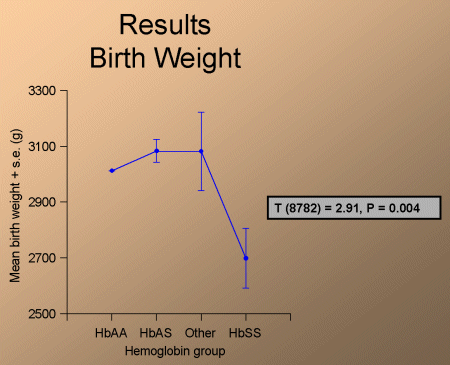 Fig. 5: Birth weights.
Fig. 5: Birth weights.
Multiple logistic regression showed that birthweight, pyelonephritis, and pregnancy-induced hypertension were the multivariate discriminators between HbAA and HbSS women.
Discussion and Conclusion
These findings are in agreement with cited and non-cited studies of pregnancy outcome in women with HbSS conducted in the last several decades. The complex of lower birth weight, pyelonephritis, and pregnancy-induced hypertension are the "defining" characteristics of this condition during pregnancy and delivery.
Advances in treatment of sickle cell disease in the last several decades has lengthened the lifespan for those suffering from SCD, and helped improve quality of life. However, much still needs to be done to alleviate the morbidity and mortality -- especially fetal loss -- associated with this condition in pregnant women.
References
- Schiliro G, et al.(1997) Presence of hemoglobinopathies in Sicily: a historic perspective. Am J Med Genet Mar 17;69(2):200-6.
- Nagel RL, Fleming AF.(1992) Genetic epidemiology of the beta S gene.Baillieres Clin Haematol Apr;5(2):331-65.
- Allison AC.(1954) Protection afforded by sickle cell trait against subtertian malarial infection. BMJ 1;290-4.
- Koshy M, et al.(1988) Prophylactic red-cell transfusions in pregnant patients with sickle cell disease: A randomized cooperative study. N Engl J Med 319:1447.
- Boletini E, et al.(1994) Sickle cell anemia, sickle cell beta-thalassemia, and thalassemia major in Albania: characterization of mutations. Hum Genet Feb;93(2):182-7
- Martin JN, Martin RW, Morrison JC.(1986) Acute management of sickle cell crisis in pregnancy. Clin Perinatol 13;853.
- Powars DR, et al.(1986) Pregnancy in sickle cell disease. Obstet Gynecol 67:217.
- Hoff C, et al.(1983) Sickle cell trait, maternal age and pregnancy outcome in primiparous women. Human Biology Dec;55(4):763-770.
- Wilkinson L. (1998) SYSTAT 8.0. Statistics. SPSS, Inc., Chicago, IL.
| Discussion Board | Previous Page | Your Poster Session |