Invited Symposium: Medicinal Plants and Drug Actions
| INABIS '98 Home Page | Your Session | Symposia & Poster Sessions | Plenary Sessions | Exhibitors' Foyer | Personal Itinerary | New Search |
Results
Studies on the effecst of aqueous plant extract on the SBP of SHR and WKY rats
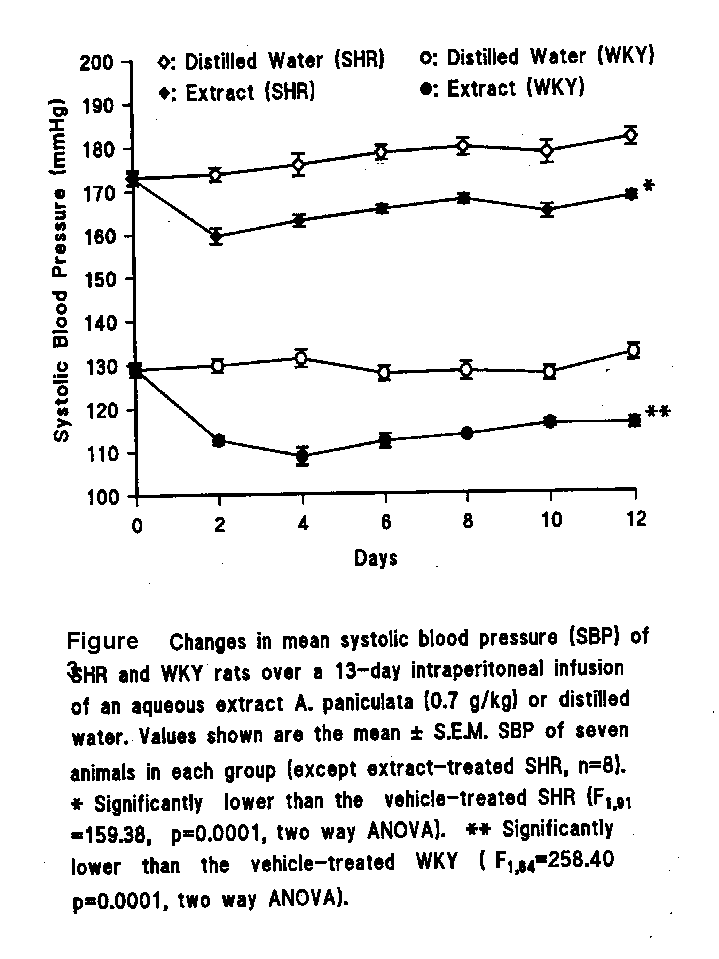
A13-day i.p. infusion of three different doses of the extract via osmotic pumps in the SHR produced significant dose-dependent reductions in the SBP, compared with vehicle-treated controls (F(3,119)=34.69, p=0.0001, two-way ANOVA). Peak reductions in SBP occurred on day 2. SBP partly recovered on day 4, but it was sustained at a lower level than that of control over the 13-day period of study (Fig. 3). From the statistical results, the lowest of the three doses was chosen as the optimum hypotensive dose of the extract. The SBP readings of the SHR and WKY rats treated with this dose were significantly lower than those of the corresponding vehicle-treated rats (F(1,91)=159.38, p=0.0001; F(1,84)=258.40, p=0.0001, two way ANOVA, respectively).
Studies on the effects of aqueous plant extract, semi-purified fractions and some pharmacological agents on the MAP of anaesthetised SD rats
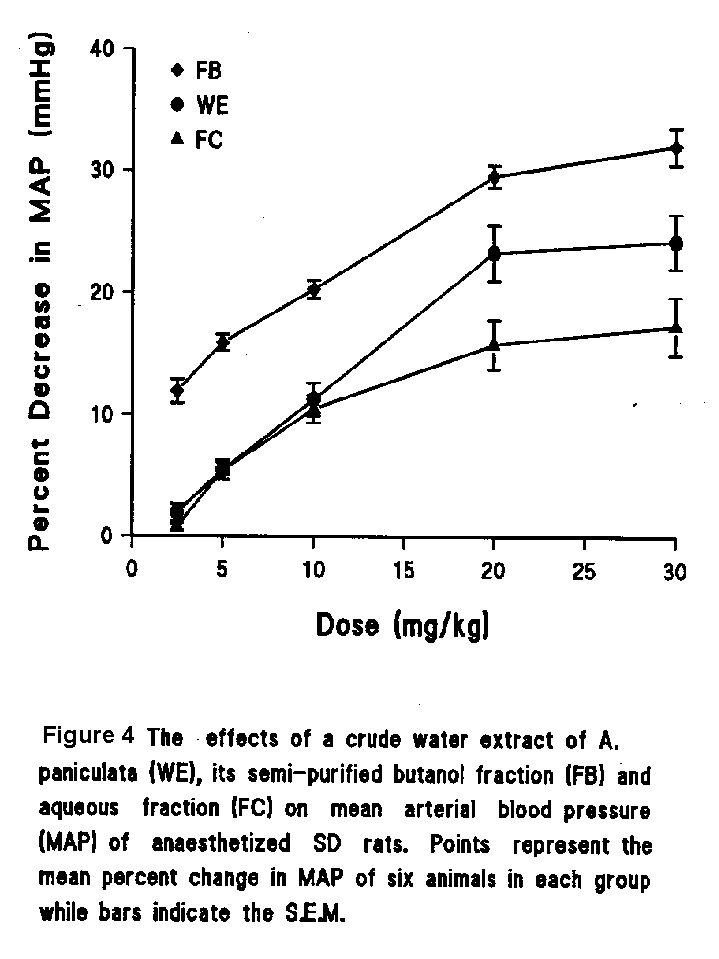
WE, FB and FC caused a significant fall in MAP in a dose-dependent manner (Fig. 4) without any significant change in HR. Their effects were brief, with the MAP returning to their original level within 4 minutes. Neither of the vehicles (normal saline and 5% DMSO in normal saline) produced any change on MAP or HR.
The hypotensive effect of FB was nearly abolished or significantly attenuated by phentolamine, an alpha-adrenergic blocker, hexamethonium, an autonomic ganglion blocker, as well as pyrilamine and cimetidine, which are H-1 and H-2 receptor blockers, respectively (Fig. 5).

The hypotensive action of FB was not affected by propranolol, atropine and captopril, which are inhibitors of beta-adrenoceptor, muscarinic cholinergic receptor and ACE respectively (Fig. 5).
Studies on the effects of DA and DDA on MAP in the anaesthetised rat
In the anaesthetized rat, DA produced a short-acting (3 minutes) and weak hypotensive effect with mean decreases of 13.0�5.0 % and 2.0� 0.9 % for MAP and HR respectively. DDA however caused a significant fall in both mean MAP and HR in a dose-dependent manner with maximum decreases of 37.6� 2.6% and 18.1� 4.8%, respectively (Fig. 6). The MAP returned to its original level within 8 min. The ED50 of DDA for MAP was 3.4 mmole/kg.
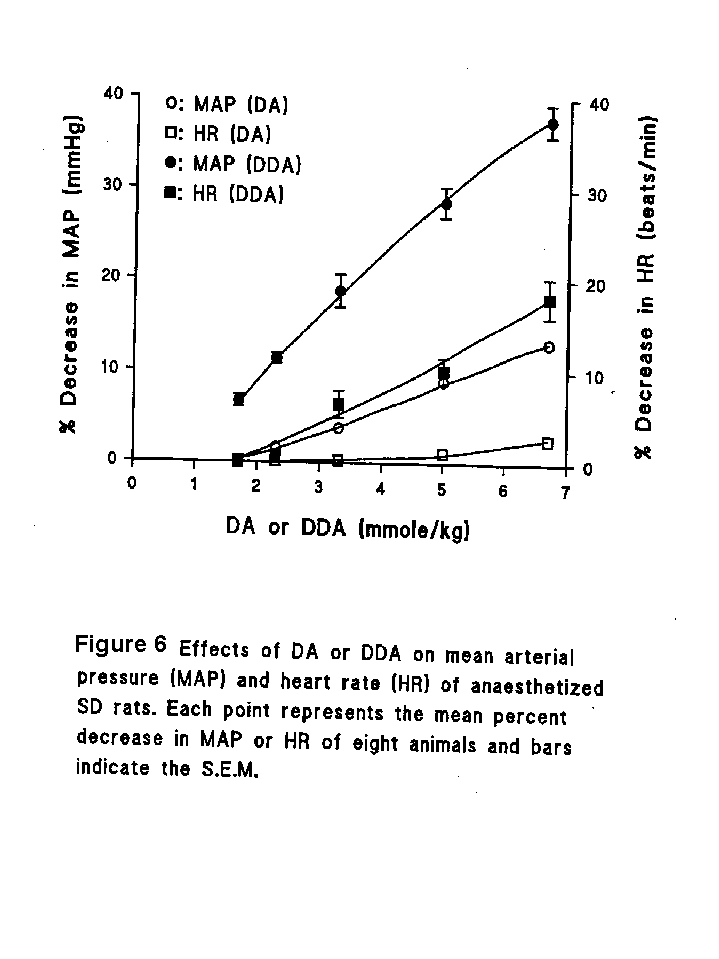
Normal saline and 5% DMSO in normal saline produced no change in MAP.
In view of the weak hypotensive activity of DA, and poor solubility at higher concentrations, pharmacological antagonist studies were subsequently done only with DDA.
Pharmacological antagonist studies with DDA in the anaesthetised rat
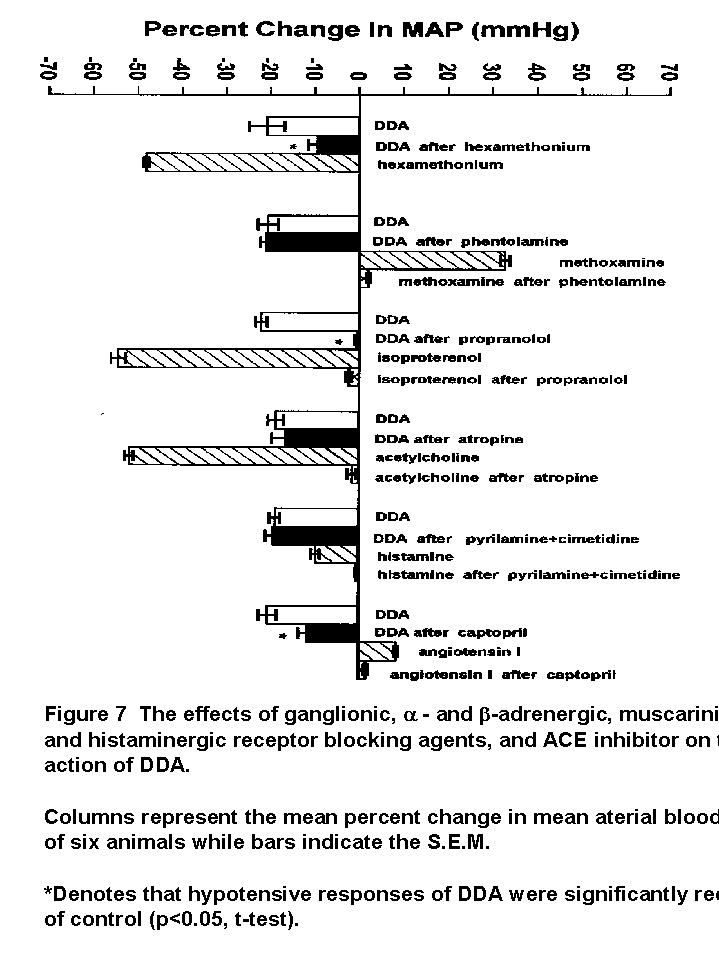
The hypotensive effect of DDA was nearly abolished or significantly attenuated by propranolol, hexamethonium, and captopril (Fig. 7).
The hypotensive action of DDA was not affected by phentolamine, atropine nor by cimetidine and pyrilamine, which are inhibitors of alpha-adrenoceptor, muscarinic cholinergic and histaminergic receptors, respectively (Fig. 7).
Studies on the effects of DA and DDA on contractions of isolated rat thoracic aortae
Effects of DA on phenylephrine- and KCl-induced contractions
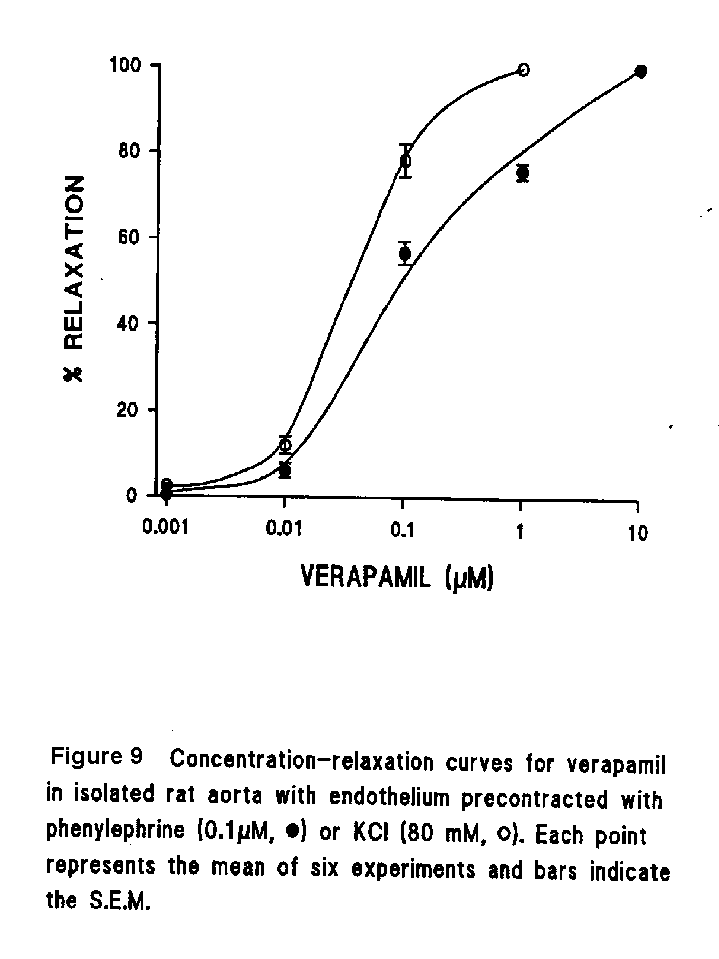
Tonic contractions induced by phenylephrine and high KCl of the rat aorta were concentration-dependently reduced by addition of DA (Fig. 8a). When experiments were carried out in rings without endothelium, the concentration-response curves were shifted to the right without modifying the maximal responses. The average initial tensions induced by phenylephrine and high KCl in endothelium-intact rings were 386�54 mg and 403 ± 56 mg, while those in endothelium-denuded rings were 427 ± 47 mg and 415 ± 44 mg, respectively. The vasorelaxant responses to DA were slow (Fig. 8a). The EC50 values were 32.9 ± 0.7µM in endothelium-intact aorta compared to 44.6 ± 0.4 micro M in the denuded aorta in phenylephrine-induced contractions, while those in KCl-induced contractions were 12.3 ± 0.2 M and 18.5 ± 0.3 micro M, respectively. The EC50 values were significantly different between endothelium-intact and denuded aortae in both phenylephrine- and KCl-induced contractions (p<0.05, t-test). The EC50 values in KCl-induced contractions were significantly lower than those in phenylephrine-induced contractions (p<0.05, t-test). Verapamil, a Ca2+-channel blocker, was also more potent in relaxing preparations contracted by KCl than by phenylephrine (Fig. 9).
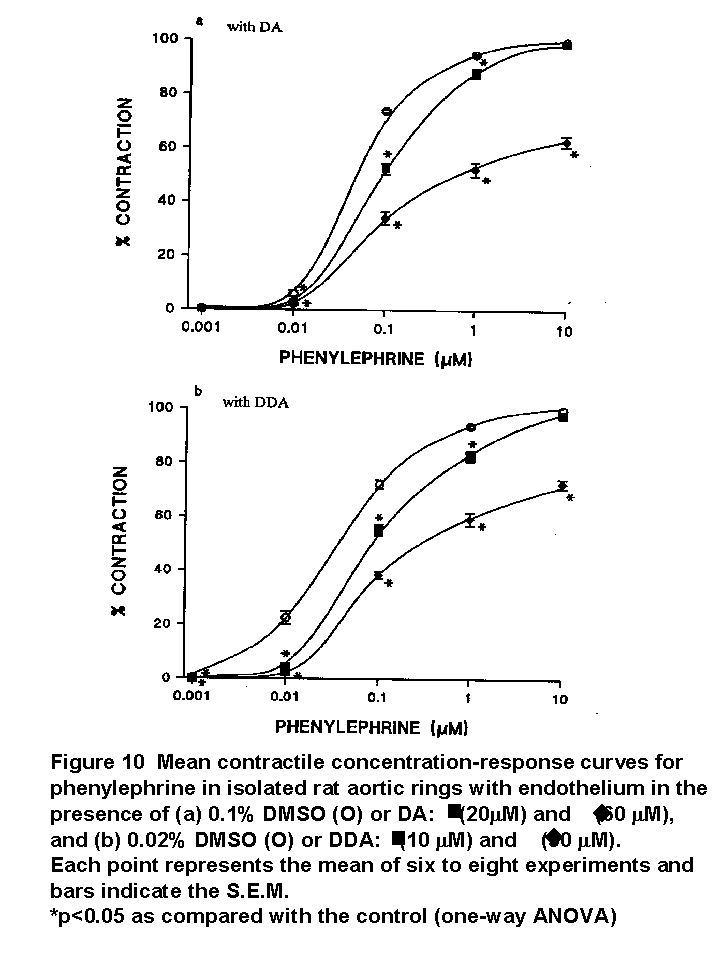
DA depressed the intensity of contractions induced by phenylephrine in a non-competitive manner (Fig. 10a).
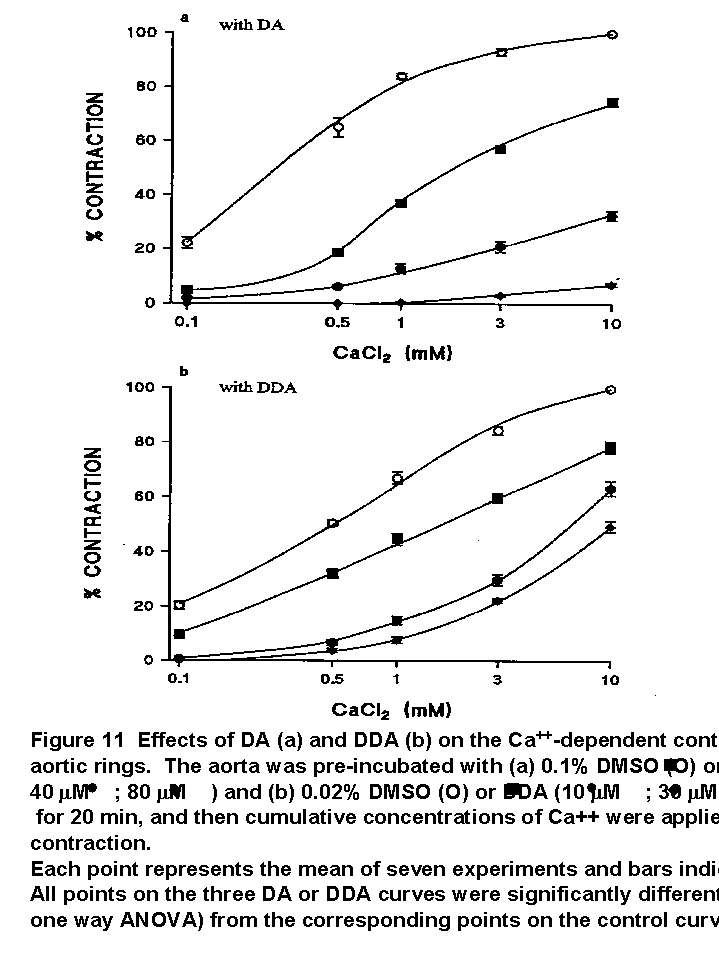
Effects of DA on Ca2+-induced contraction in the presence of high K+
In Ca2+-free solution containing 55 mM K+, the addition of Ca2+ caused a stepwise increase of contraction in the rat aorta. After pre-treatment for 20 min, DA inhibited this contraction in a concentration-dependent manner (Fig. 11a).
Effects of DA on caffeine- and norepinephrine-induced contractions
Caffeine caused a rapid phasic contraction of the aortic ring in Ca2+-free medium. The contractions were inhibited by DA in a concentration-dependent manner and were almost completely abolished at the concentration of 120 micro M (Fig. 12).
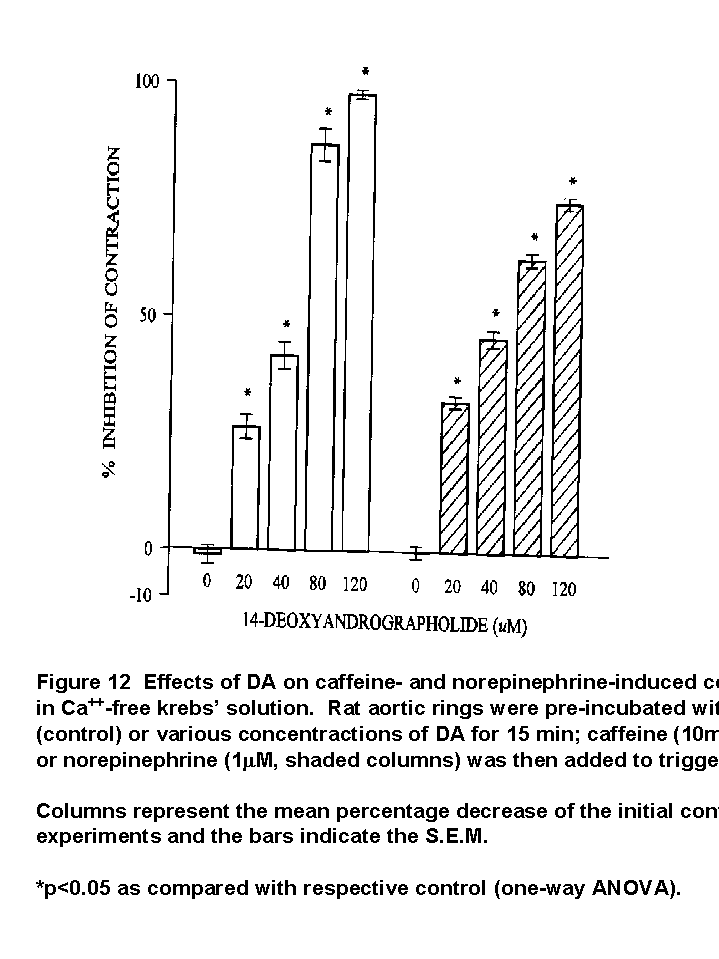
Norepinephrine induced a phasic contraction followed by a tonic contraction in Ca2+-free solution. DA similarly inhibited this contraction, but to a lesser extent compared to its action on caffeine-induced contraction (Fig. 12).
Effects of L-NAME, methylene blue, indomethacin and glibenclamide on the relaxant activity of DA
Prior incubation of the preparations with (a) L-NAME and (b) methylene blue for 20 min caused rightward shifts of the relaxant concentration-response curves for DA in preparations contracted by phenylephrine, but it did not produce significant shift in preparations contracted by KCl (Fig. 13a and 13b). In the presence of L-NAME and methylene blue, the average initial tensions induced by phenylephrine were 586�52 mg and 531�60 mg while those remained unchanged in KCl-induced contraction (405�53 mg). EC50 values of DA in control rings (38.8�0.4. microM for L-NAME and 34.1�0.4 microM for methylene blue) and in rings preincubated in L-NAME (50.0�0.3 microM) or methylene blue (50.1�0.4 micro M) were significantly different in phenylephrine-induced contractions (p<0.05, t-test). There were no significant differences between EC50 values in control rings (14.4�0.3 micro M for L-NAME and 12.7�0.8 microM for methylene blue) and those in rings preincubated in L-NAME (14.2�0.5 microM) or methylene blue (14.1�0.7 micro M) in KCl-induced contractions (p>0.05, t-test).
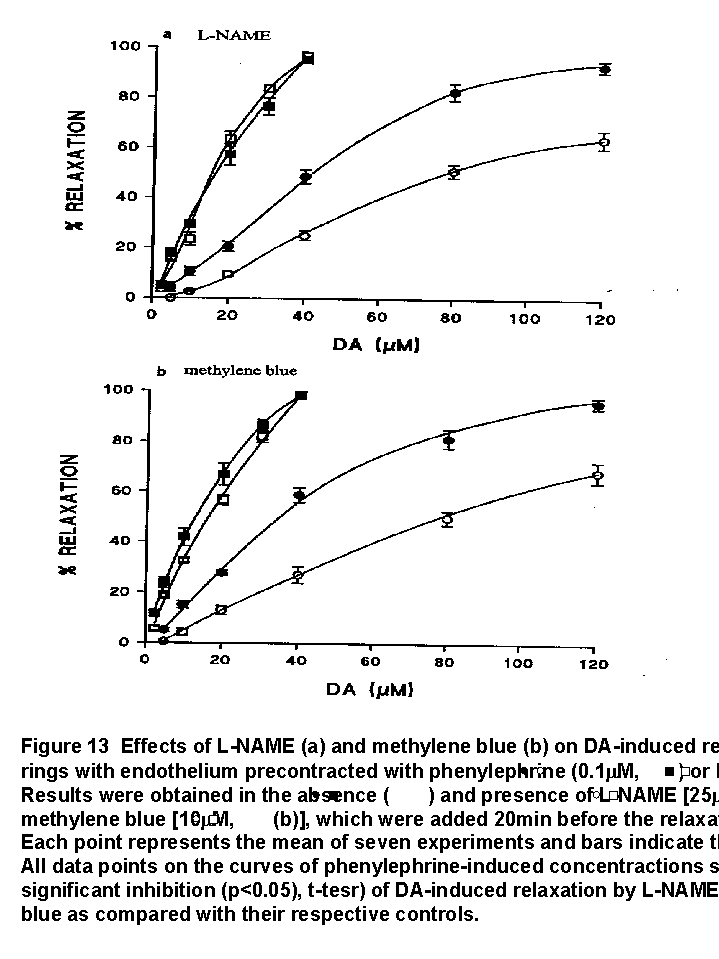
Indomethacin and glibenclamide did not interfere with DA-induced vasorelaxation in preparations precontracted with phenylephrine (data not shown).
Effects of DDA on phenylephrine- and KCl-induced contractions
Tonic contractions induced by phenylephrine and high KCl of the rat aorta were also concentration-dependently reduced by addition of DDA (Fig. 8b). The concentration-response curves of DDA were shifted to the right when experiments were carried out in rings without endothelium. The average initial tensions induced by phenylephrine and high KCl in endothelium-intact rings were 394 ± 51 mg and 403 ± 52 mg, while those in endothelium-denuded rings were 435 ± 48 mg and 418 ± 46 mg, respectively. The vasorelaxant reponses to DDA were slow (Fig. 8b). The ED50 values of DDA were 13.2 ± 0.6 micro M/L in endothelium-intact aorta compared to 18.9 ± 0.3 micro M/L in the denuded aorta in phenylephrine-induced contractions, while those in KCl-induced contractions were 12.6 ± 0.4 micro M/L and 14.9 ± 0.3 micro M/L, respectively. The ED50 values were significantly different between endothelium-intact and denuded aortae in both phenylephrine- and KCl-induced contractions (p<0.05, t-test). The ED50 values of phenylephrine- and KCl-induced contractions were not significantly different in endothelium-intact aorta (13.2 ± 0.6 micro M/L and 12.6 ± 0.4 micro M/L, respectively; p>0.05, t-test). The ED50 value in phenylephrine-induced contractions was significantly greater than that in KCl-induced contractions in endothelium-denuded aorta (18.9 ± 0.3 micro M/L and 14.9 ± 0.3 micro M/L, respectively; p<0.05, t-test).
DDA depressed the intensity of contractions induced by phenylephrine in a non-competitive manner (Fig. 10b).
Effects of DDA on Ca2+-induced contraction in the presence of high K+
In Ca2+-free solution containing 55 mM K+, the addition of Ca2+ caused a stepwise increase of contraction in the rat aorta. After pre-treatment for 20 min, DDA inhibited this contraction in a concentration-dependent manner (Fig. 11b).
Effects of DDA on caffeine- and norepinephrine-induced contractions
Caffeine and norepinephrine caused a rapid phasic contraction or a phasic contraction followed by a tonic contraction in Ca2+-free solution. Both these transient contractions were not affected by DDA (data not shown).
Effects of L-NAME, methylene blue, indomethacin and glibenclamide on the relaxant activity of DDA
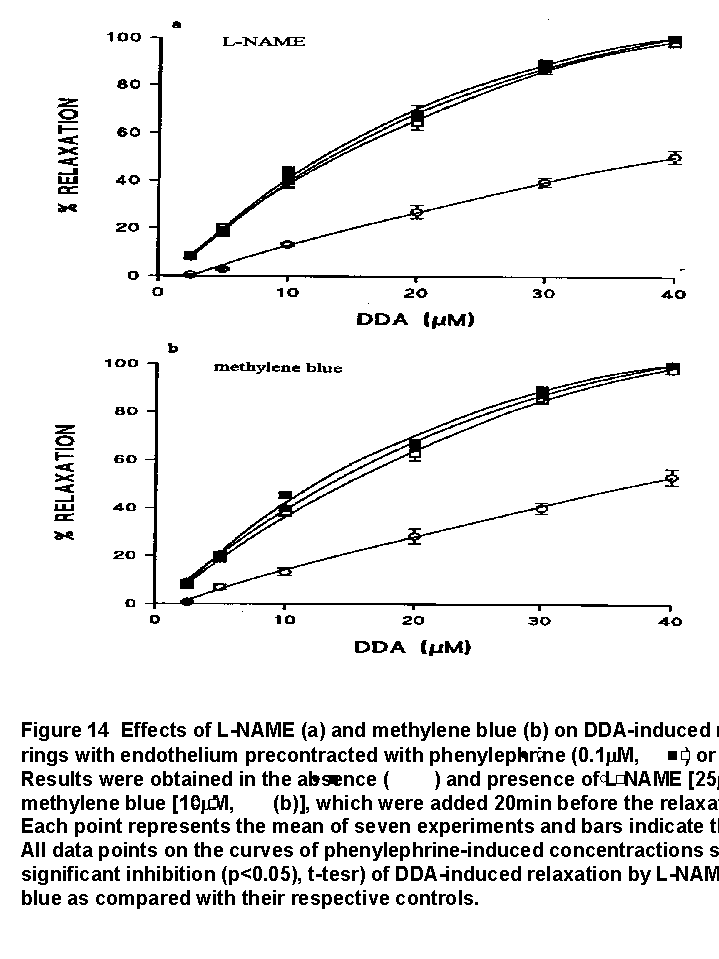
Prior incubation of the preparations with (a) L-NAME and (b) methylene blue for 20 min caused significant rightward shifts of the relaxant concentration-response curves for DDA in preparations contracted by phenylephrine, but did not produce significant shift in preparations contracted by KCl (Fig. 14a and 14b). In the presence of L-NAME and methylene blue, the average initial tensions induced by phenylephrine were 591 ± 54 mg and 538 ± 60 mg while these remained unchanged in KCl-induced contraction (404 ± 53 mg). ED50 values of DDA in control rings (12.8 ± 0.2 micro M/ l for L-NAME and 13.1 ± 0.3 micro M/L for methylene blue) and in rings preincubated in L-NAME (19.1 ± 0.4 micro M) or methylene blue (19.0 ± 0.6 micro M/L) were significantly different in phenylephrine-induced contractions (p<0.05, t-test). There were no significant differences between ED50 values in control rings (12.4± 0.5 micro M/L for L-NAME and 12.8 ± 0.8 micro M/L for methylene blue) and those in rings preincubated in L-NAME (13.1± 0.5 micro M/L) or methylene blue (14.1 ± 0.7 µM) in KCl-induced contractions (p>0.05, t-test).
Indomethacin and glibenclamide did not interfere with the DDA-induced vasorelaxation in preparations precontracted with phenylephrine (data not shown).
Studies on the cardiac effects of DDA on isolated right atria
At the start of the experiments, the atrial preparations contracted at the rate of approximately 180 beats/min.
Treatment of test tissues with DDA (5-320 micro M/L) caused a concentration-dependent decrease in the rate of atrial beating, while the rate in vehicle-treated atria (DMSO less than 0.16%) remained relatively constant (Fig. 15).
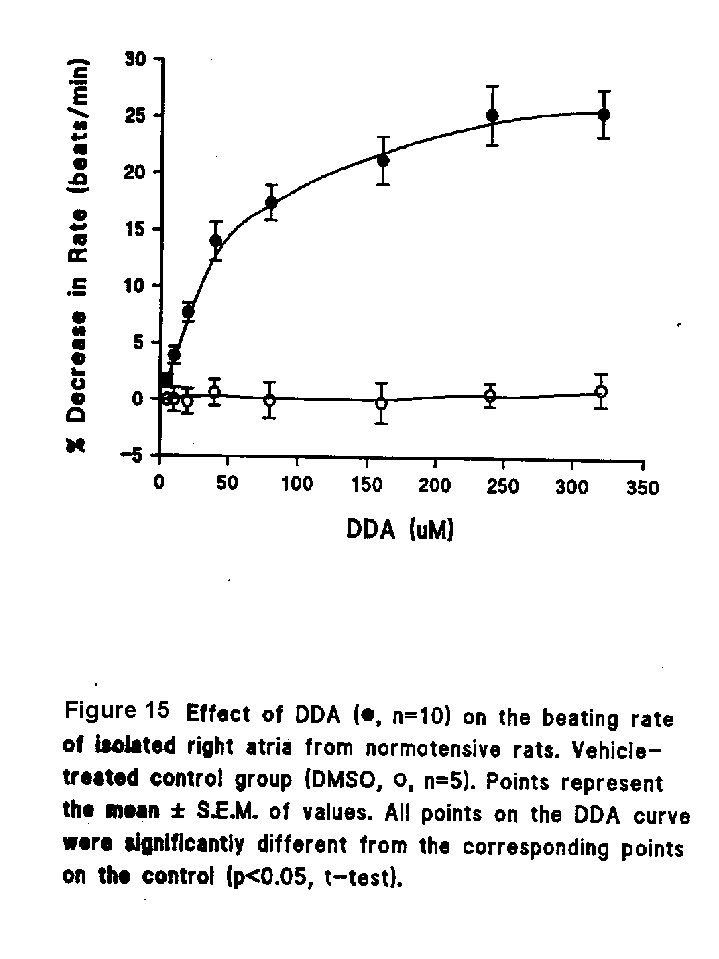
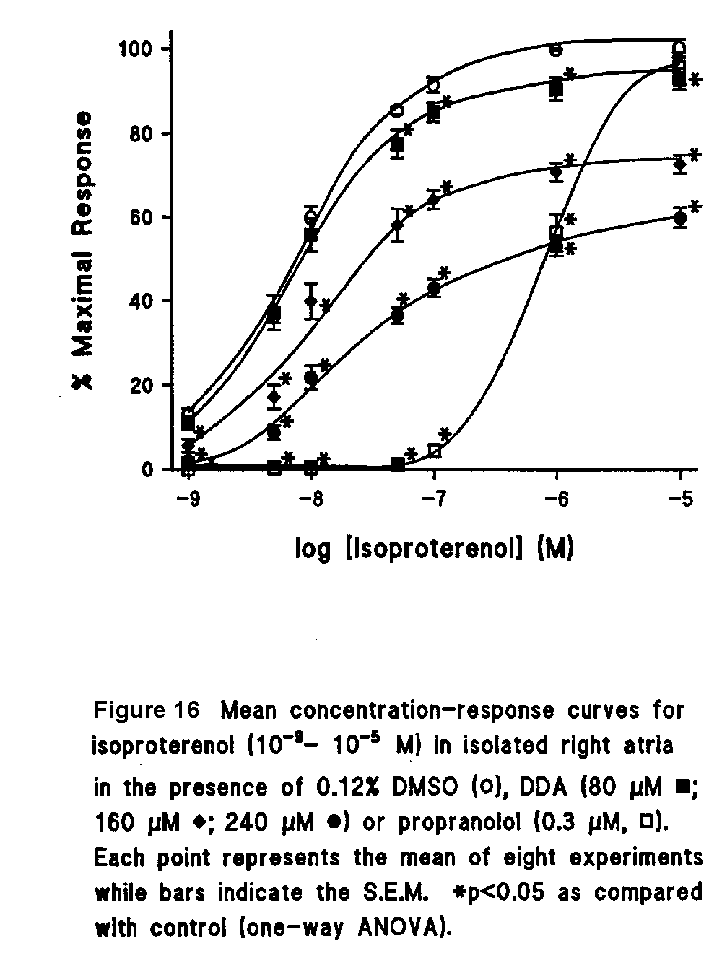
DDA (80-240 micro M/L) shifted the concentration-response curve of isoproterenol to the right in a dose-dependent manner and significantly decreased the maximum response to isoproterenol. The dose-response curve of isoproterenol was also shifted to the right by propranolol but without a significant change in the maximal response (Fig. 16).
| <= Materials & Methods | RESULTS | Discussion & Conclussions => |
| Discussion Board | Next Page | Your Symposium |